Month 10
HOW RACISM AFFECTS OUR HEALTH

Month 10 Challenge
Inequalities are exacerbated by the pandemic. Households of all ages, genders, races, and ethnicities, and households in rural, urban, and suburban areas, are all impacted by the COVID-19 pandemic. But sheltering in place is a luxury that many ALICE families cannot afford. Differences in income and savings play a role in who can stay home, buy protective gear and essential items, take time off work when sick, and access quality health care.
The COVID-19 pandemic has shed light on the disproportionately high number of deaths in the black community. New statewide data is exposing racial fault lines among people who die from COVID-19 and those who don’t, 42% of deaths in the first months of the pandemic afflicting Black Illinoisans even though they represent just 15% of the population. In Chicago, black residents make up about 29% of the city’s population, however 72% of the city’s residents who died from COVID-19 at the onset of the pandemic were black. And according to the public health commissioner, 52% of those testing positive were black.
Health care leader, Brenda Battle, vice president of University of Chicago Medicine’s Urban Health Initiative and its chief diversity, inclusion and equity officer stated, “I think that health care has realized that the impact that COVID has had on black and brown communities is not happenstance, that long years of compounding health care disparities, structural issues, policies that are basically racist policies that impeded equity in our organizations, are a reality. We have to realize that we have contributed to these realities and we have to do our part in addressing them.”
You may have heard about the wealth gap, but have you heard about the wealth-health gap? According to the NY Times 1619 Project, “racial health disparities are foundational as democracy itself.” Socioeconomic status and institutional racism lead to disparities across living conditions, limit access to quality health care, and contribute to chronic stress. These factors lead to shorter life spans and higher likelihood of adverse health outcomes for people living in poverty and people ofIn Illinois, we are seeing how race and income can disproportionately impact individuals’ health. Importantly, the studies cited below illustrate that this is not a result of individual choices, but rather institutional racism:
Published in the journal, Nature, a recent study found that millions of black people have been affected by racial bias in health-care algorithms used by many U.S. hospitals, resulting in black people being less likely than white people who were equally sick to be referred to programs that aim to improve care for patients with complex medical needs.
A study by the American Bar Association notes that “the poverty in which black people disproportionately live cannot account for the fact that black people are sicker and have shorter life spans than their white complements…racial and ethnic minorities receive lower-quality health care than white people—even when insurance status, income, age, and severity of conditions are comparable.”
Please choose two or more of the below activities to complete:
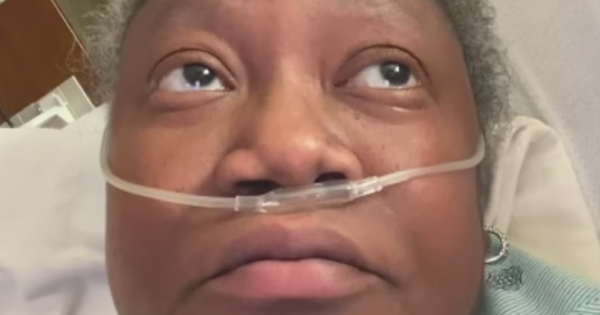
ACTIVITY 1
Read the story about the recent COVID-19 death of Dr. Moore and the racial bias it demonstrates in the U.S. health care system.
Select
ACTIVITY 2
Hear Dr. Camara Phyllis Jones explain social determinants of health through her analogy of the “cliff of good health” in a video collaboration with the Urban Institute.
Select
ACTIVITY 3
Watch David. R Williams, a public health sociologist, on the TED stage discuss why race and deep-rooted systemic racism have such a profound impact on health.
Select
ACTIVITY 4
Check Out this Fact Sheet from the American Psychological Association exploring the compounding impact of socioeconomic status and race on health.
Select
ACTIVITY 5
Hear the story of Henrietta Lacks, an African American woman whose cells have been used to test the effects of radiation and poisons, to study the human genome, to learn more about how viruses work, and played a crucial role in the development of the polio vaccine. It is most important to note that, while Ms. Lacks’ cells have been the source of life-saving medical solutions, no consent was obtained to culture her cells, nor were she or her family compensated for their extraction or use.
Select


